- Have any questions?
- +91 90084 82284
- info@drsridharpsoncologist.com
Types of Radiation Therapy: Treatments, Therapies & Applications

Chemotherapy for Brain Tumor: An Effective Treatment Modality
June 15, 2023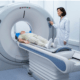
An Insight into Radiation Therapy Machines
July 24, 2023Cancer. It is a powerful foe that instills fear in the minds of millions of people worldwide. We experience a mixture of terror, pain, and helplessness at the mere mention of the term, sending shivers down our spines. Radiation therapy is a potent weapon that shines a glimmer of light amid this darkness. Radiation therapy is a powerful tool in the battle against this unrelenting illness, trying to kill cancer cells and provide relief to individuals under its control.
“Radiation therapy has completely changed how cancer is treated, thanks to its capacity to accurately target and destroy tumors,” says Dr. Sridhar PS, a renowned radiation oncologist in India.
This blog aims to shed light on the complex web of radiation treatments by explaining the different types of radiation therapy and modalities used in the fight against cancer.

Types of radiation for cancer
External radiation therapy, or external beam radiation therapy (EBRT)
EBRT is the most common form of radiation therapy. EBRT is a noninvasive treatment often given over several weeks in numerous sessions. It includes creating high-energy radiation beams that are aimed at the tumor from outside the body using a device known as a linear accelerator. The radiation beams are precisely shaped and focused on minimizing exposure to healthy tissues while accurately striking the tumor. This sort of therapy is adaptable and effective in treating various cancers, including lung, breast, prostate, and head and neck tumors.
“External radiation therapy is now more precise and successful because of cutting-edge methods like IMRT and stereotactic body radiation therapy (SBRT),” explains Dr. Sridhar PS, a doctor with expertise in CyberKnife Treatment in India. “EBRT allows for customized treatment plans and improved patient results.”
Brachytherapy, or internal radiation therapy
Internal radiation therapy or brachytherapy entails placing radioactive sources inside or close to the tumor. This minimizes exposure to nearby healthy tissues while enabling accurate radiation delivery. Depending on the circumstance, brachytherapy may be applied using either temporary or permanent implants. This method gives a concentrated dosage of radiation directly to the target area, making it particularly efficient for localized tumors like prostate, cervical, or breast cancer. It may be used alone or in conjunction with other therapies, such as surgery or external beam radiation therapy, to increase effectiveness and restrict tumor growth.

Radiotherapy types and their uses
The various types of radiation treatment include:
| Radiation therapy | Description | Cancer Type |
| Three-dimensional conformal radiation therapy (3DCRT) | Three-dimensional conformal radiation therapy (3DCRT) customizes radiation treatment for each patient using CT scans. The goal is to deliver radiation precisely to the tumor while minimizing damage to nearby healthy tissue. | – Prostate Cancer – Breast Cancer – Lung Cancer often for non-small cell lung cancer (NSCLC) – Head and Neck Cancers (e.g., nasopharyngeal cancer, laryngeal cancer, or oral cavity cancers) – Gastrointestinal Cancers (e.g., rectal cancer, anal cancer, and esophageal cancer) – Brain Tumors |
| Intensity-modulated radiation therapy (IMRT) | During IMRT treatment, the treatment machine’s built-in shielding moves while the radiation beam is active, allowing intentional variation of the radiation dose. Multiple beams from different directions precisely sculpt the radiation dose to match the tumor’s shape. It is the most common radiotherapy for prostate cancer. | – Head and Neck Cancers (e.g., oral cavity cancer, pharynx, and larynx) – Prostate Cancer – Breast Cancer – Gynecological Cancers (e.g., cervical, endometrial, and vaginal cancers) – Lung Cancer (often in cancers close to critical structures like the spinal cord) – Central Nervous System (CNS) Tumors |
| Volumetric modulated arc therapy (VMAT) | Volumetric modulated arc therapy (VMAT) delivers a continuous radiation dose, similar to IMRT, by varying the radiation dose during treatment while the treatment machine rotates. It precisely shapes the radiation dose to the tumor while minimizing exposure to surrounding organs. | – Head and Neck Cancers (e.g., oral cavity, pharynx, larynx) – Prostate Cancer – Gastrointestinal Cancers (e.g., rectal cancer, anal cancer, and stomach cancer) – Lung Cancer (often in cases of proximity to the heart or spinal cord) – Central Nervous System (CNS) Tumors Breast Cancer |
| Image-guided radiation therapy (IGRT) | Image-guided radiation therapy (IGRT) enhances the accuracy and precision of treatment by utilizing X-ray images taken right before, during, or after radiation therapy sessions. | – Prostate cancer – Head and neck cancers (e.g., oral cavity, pharynx, larynx) – Lung cancer – Breast cancer – Gastrointestinal cancers (e.g., rectal cancer, anal cancer) – Gynecological cancers (e.g., cervical cancer, endometrial cancer) Brain tumors – Sarcomas (soft tissue and bone) – Genitourinary cancers (e.g., bladder cancer, testicular cancer) Lymphomas Pediatric cancers |
| Stereotactic radiosurgery (SRS) and stereotactic radiotherapy (SRT) | SRS and SRT are noninvasive procedures that deliver high doses of radiation without anesthesia or incisions. They maximize radiation dose to the targeted area while minimizing exposure to healthy brain tissue. SRS is typically administered in a single treatment, while SRT is delivered over multiple treatments. | – Brain Tumors (e.g., gliomas and meningiomas) Spine Tumors – Early-stage lung cancers – Liver Cancer – Prostate Cancer – Pancreatic Cancer |
| Brachytherapy, or internal radiation therapy | In brachytherapy, the radioactive sources, enclosed in protective capsules, are guided to the cancerous area through specialized applicators. In some cases, the radiation sources may be implanted into an organ during a surgical procedure. | – Prostate Cancer – Gynecological Cancers (e.g., cervical cancer, endometrial cancer, and vaginal cancer) Breast Cancer – Head and Neck Cancers (e.g., oral cavity and nasopharyngeal) – Skin Cancer – Lung Cancer – Eye Cancer Soft tissue cancers |
| Superficial X-ray radiation therapy (SXRT) | Superficial X-ray radiation therapy (SXRT) utilizes low-penetrating X-rays to treat skin cancers effectively. These X-rays are specifically designed to target the surface layers of the skin, making them highly effective in treating skin cancer. | – Non-melanoma skin cancers arising from the outer layers of the skin – Cutaneous Lymphoma – – Dermatofibrosarcoma – Protuberans (Cancer in the deep layers of the skin) – Basal cell carcinomas (BCC) (Skin cancer of the outermost layer) – Squamous cell carcinomas (SCC) – Kaposi’s sarcoma |
| Intraoperative radiation therapy (IORT) | Intraoperative radiation therapy (IORT) is a precise radiation technique delivered directly into the surgical cavity during cancer removal surgery. It utilizes a specialized radiation therapy machine to administer the required radiation dose during the procedure. | – IORT is suitable for select cases of early-stage breast cancer, particularly in older and lower-risk individuals. |
If you seek effective cancer treatment options, please consult Dr. Sridhar PS. He is a highly skilled cancer specialist in various cancer treatment techniques, including Immunotherapy.
Benefits of Radiation therapies
Different radiation therapies offer unique benefits based on treatment goals and patient factors.
| Radiation Therapy | Benefits |
| Three-dimensional conformal radiation therapy (3DCRT) | Precise targeting, reducing side effects. |
| Intensity-modulated radiation therapy (IMRT) | Customizable dose, organ preservation. |
| Volumetric modulated arc therapy (VMAT) | Faster treatment and improved dose conformity. |
| Image-guided radiation therapy (IGRT) | Enhanced accuracy and adaptability. |
| Stereotactic radiosurgery (SRS) and stereotactic radiotherapy (SRT) | High precision, noninvasive. |
| Brachytherapy | Targeted radiation, shorter treatment duration. |
| Superficial X-ray radiation therapy (SXRT) | Precise targeting, shorter treatment sessions. |
| Intraoperative radiation therapy (IORT) | Convenient and streamlined treatment, enhanced tumor control. |
“Benefits depend on cancer type, stage, and patient health,” says radiotherapy expert Dr. Sridhar PS. “Medical evaluation is crucial for individualized treatment decisions.”
Risks & possible side effects
Potential side-effects may include:
- Infection: Chemotherapy-induced neutropenia can increase susceptibility to infections due to a reduction in the number of neutrophils in the bloodstream.
- Fatigue: Chemotherapy-related fatigue typically starts within 24-48 hours of treatment, and it may take 3-4 months after treatment to recover energy levels.
- Shortness of breath: Chemotherapy drugs or lung-focused radiation therapy can cause shortness of breath, often due to reduced oxygen in the blood (anemia).
- Nausea and vomiting: Cancer patients can experience nausea either due to the disease or as a side effect of treatments, such as chemotherapy.
- Loss of appetite: Various factors such as pain, gastrointestinal symptoms, changes in taste preferences, and emotional distress like depression, anxiety, and stress related to cancer and its treatment can contribute to a loss of appetite and diminished interest in food.
- Weight loss: Weight loss in individuals with cancer can occur due to multiple side effects of the disease and its treatments, including fatigue, nausea, vomiting, constipation, diarrhea, mouth issues, altered taste, and diminished appetite.
Please consult your doctor as soon as possible if you have any side-effects mentioned above or are apprehensive about any other sensations post-treatment.

Post-operative care
Here are the key points for post-operative care after cancer radiation therapy, presented as bullet points:
- Wound care: Follow instructions to prevent infection and promote healing.
- Pain management: Take prescribed pain medications and follow pain relief techniques recommended by your healthcare provider.
- Side effect management: Address and manage side effects such as fatigue, skin changes, nausea, and digestive issues with guidance from your healthcare team.
- Follow-up appointments: Attend regular follow-up appointments to monitor progress, evaluate treatment efficacy, and discuss any new symptoms or concerns.
- Emotional support: Seek emotional support from loved ones, support groups, counselors, or therapists to cope with the emotional challenges of cancer treatment.
- Healthy lifestyle: Adopt a nutritious diet, engage in physical activity within recommended limits, prioritize rest, and avoid harmful habits like smoking or excessive alcohol consumption.
If you or a loved one is living with cancer and wish to explore advanced techniques in radiation therapy, please contact Dr. Sridhar PS. With almost 20 years of experience and having treated over 10000 patients, he is among the preferred radiation oncologists in India.
